After confirming that the facial nerve was not on the dorsal surface of the cerebellopontine angle tumour, using a facial stimulator-monitor designed by us, 13 internal decompression of the large extrameatal tumour was undertaken with an ultrasonic surgical aspirator (CUSA EXcel, Vallylab, Boulder, Colorado, USA). The microsurgical removal of the tumours comprised three steps: cytoreduction of the large extrameatal cerebellopontine angle portion of the tumour, the removal of the intrameatal tumour, and the removal of the last lump of tumour remaining in the extrameatal region just outside the porus acusticus. The foramen magnum was not usually opened. Irrespective of the tumour size, a retrosigmoid suboccipital craniotomy of 5 cm length and 4 cm width was made to expose the posterior part of the sigmoid sinus and the inferior part of the transverse sinus.
#PORUS ACOUSTICUS SKIN#
A longer incision placed more medially was used in patients with short thick necks, while a shorter skin incision placed more laterally was used in those with long thin necks. A curvilinear skin incision of 12 cm length was placed 3–4 cm posterior to the mastoid. Surgical procedureĪll operations were done by single neurosurgeon (IY), using the retrosigmoid suboccipital transmeatal approach in the lateral position. Patients with neurofibromatosis type 2 or with a recurrent tumour were excluded from the study. In this study we analysed the 50 patients with large tumours. The extrameatal diameter of the tumours was ⩾3 cm in 50 of the 89 tumours ( large 56%), and <3 cm in 39 ( small to medium 44%). The subjects consisted of 89 consecutive patients with unilateral acoustic neurinomas in the period from 1992 to 2001.

Very favourable results can be obtained using the retrosigmoid approach for the removal of large acoustic neurinomas. All but two patients (96%) had a good functional outcome.Ĭonclusions: The method resulted in a high rate of functional facial nerve preservation, a low incidence of complications, and good functional outcomes, with no mortality and minimal morbidity. Cerebrospinal fluid leak occurred in 4%, but there were no cases of meningitis. One patient recovered useful hearing after tumour removal. The facial nerve was anatomically preserved in 92% of the patients and 84% had excellent facial nerve function (House-Brackmann grade 1/2). The tumour was removed completely in 43 of 50 patients (86%). Results: There were no postoperative deaths. The last pieces of tumour were removed by sharp dissection from the facial nerve bidirectionally, and resected cautiously in a piecemeal fashion.
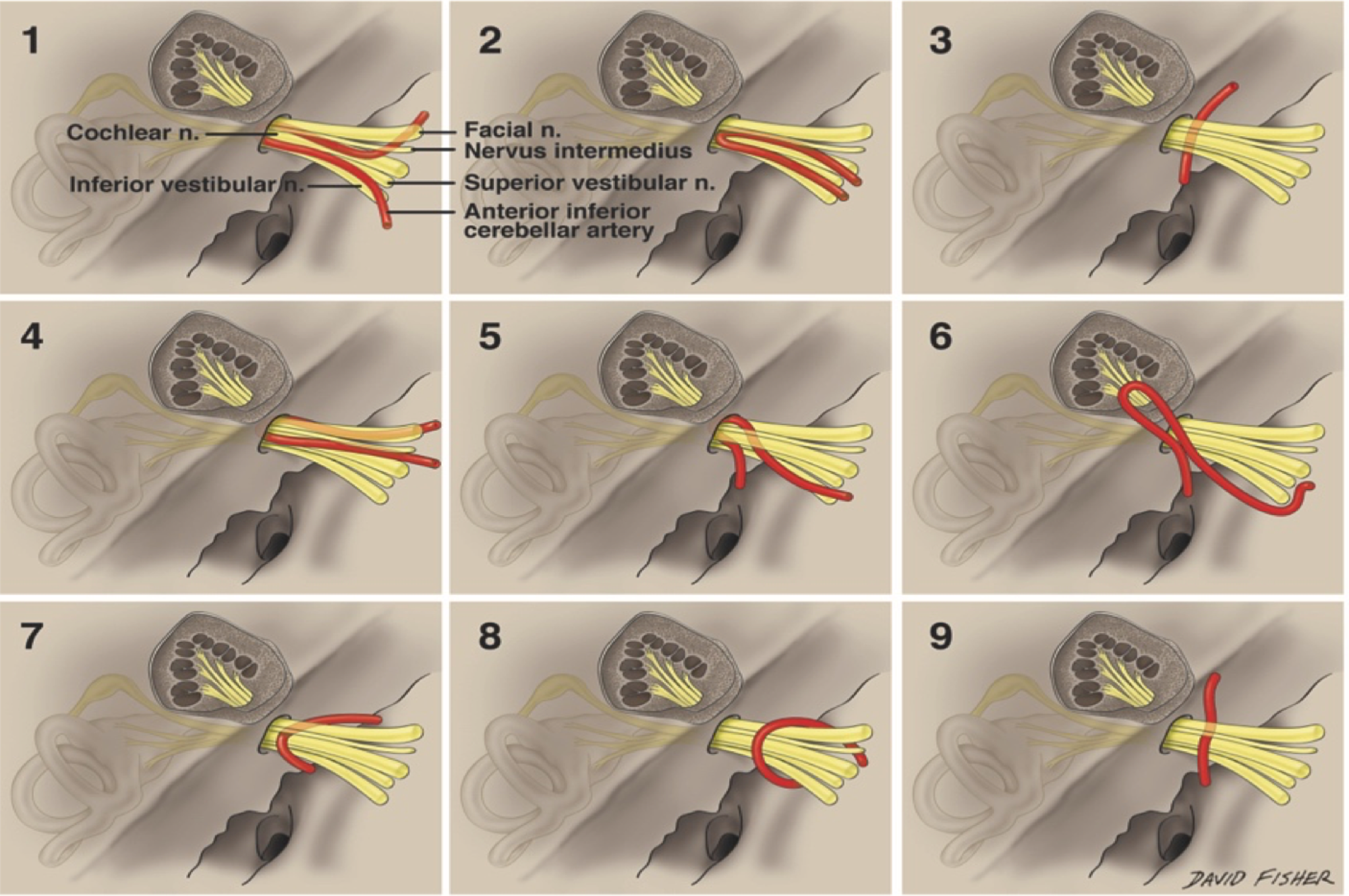
Excision began with the large extrameatal portion of the tumour, followed by removal of the intrameatal tumour, and then removal of the residual tumour in the extrameatal region just outside the porus acusticus.
Methods: Large acoustic neurinomas (mean (SD), 4.1 (0.6) cm) were removed from 50 consecutive patients by the retrosigmoid suboccipital approach while monitoring the facial nerve using a facial stimulator-monitor.

Objective: To evaluate the safety and efficacy of removing large acoustic neurinomas (⩾3 cm) by the retrosigmoid approach.
